First….. in ER Nishitarumizu 2001.3.13
Seizure
・詳細な病歴で本当にSeizureかどうかを見極める.
発症前 Trigger, aura (Simple Partial Seizure), abrupt onset nonspecific
発作時 Local or generalized? symmetrical? Progression of motor activity, incontinence
発作後 Postictal state, Todd’s paralysis 1-2 minutes duration, lack of recall
Differential diagnosis
Syncope - rapid recovery, no post-ictal like symptoms
Pseudoseizure - side-to-side head thrashing, rhythmic pelvic thrusting
Clonic extremity alternating motions,
no incontinence,injury, post-ictal like symptoms,lactic acidosis
Hyperventilation gradual onset, anxiety, reproduce
Movement disorder
Migraine
Narcolepsy/cataplexy

※Secondary seizure(原因治療が優先)を見逃さない!
Causes of secondary seizures
Intracranial hemorrhage (subdural,epidural,subarachnoid,intraparenchymal)
Structural abnormalities
Vascular lesion (aneurism,arteriovenous malformation,vasculitis)
Mass lesions (primary or metastatic neoplasms)
Degenerative diseases
Congenital abnormalities
Trauma (recent or remote)
Infection (meningitis,encephalitis,abscess,HIV encephalopathy, CJD, syphilis)
Metabolic disturbances
Hypo-or hyperglycema
Hypo-or hypernatremia
Heperosmolar states
Uremia
Hepatic failure
Hypocalcemia,hypomagnesemia (rare)
Pellagra
Toxins and drugs (many)
Cocaine, amphetamine, heroin
Lidocaine, salicylates, ergot, digitalis, Erythropoietin,Cyclospporin
Antidepressants
Theophiline, penicillins and b-lactam antibiotics, Quinolones, INH
Alcohol withdrawal
Drug withdrawal (Barbiturate,Benzodiazepine
Eclampsia of pregnancy (may occur up to eight weeks postpartum)
Hypertensive encephalopathy
Anoxic-ischemic injury (cardiac arrest ,sever hypohemia)
Reduced cerebral blood flow (hypotension,Adams-Stokes)
・画像は必要か?
ACEP recommendations for obtaining emergent neuroimaging following a seizure
New focal deficits
Persistent altered mental status
Recent head trauma
Fever
Anticoagulation therapy
History of cancer
Persistent or sever headache
Change in seizure pattern
Suspicion of AIDS (Neurology)
Age >40 (option Neurology)
Partial-onset seizure (option Neurology)
Unknown cause (urgent indication Neurology)


・入院させるか?帰すか?抗痙攣剤を出すか?
ACEP guidelines for hospital admission of patients with new-onset seizure
Persistent altered mental status
CNS infection
New intracranial lesion
Underlying correctable medical problem
Significant hypoxia
Hypoglycemia
Hyponatremia
Dysrhysmia
Significant alcohol withdrawal
Acute head trauma
Status epilepticus
Eclampsia
※The most important predictors of the risk of recurrence were the etiology
and the results of the EEG
※Idiopathic seizure,normal neurological exam, EEG normal : 24%(recurrent within 2years)
,EEG abnormal : 48%
Abnormal neurological exam, EEG normal : 48%
,EEG abnormal:65%
・神経所見に異常があったり、画像上の異常がある場合は抗痙攣剤を開始する.
治療可能な二次性痙攀ではその治療のみ行なう.
原因不明の場合はrisk/benefitを説明し、内服を持たさずに一週間以内に神経内科を受診させて
も良いのでは?(controversial)
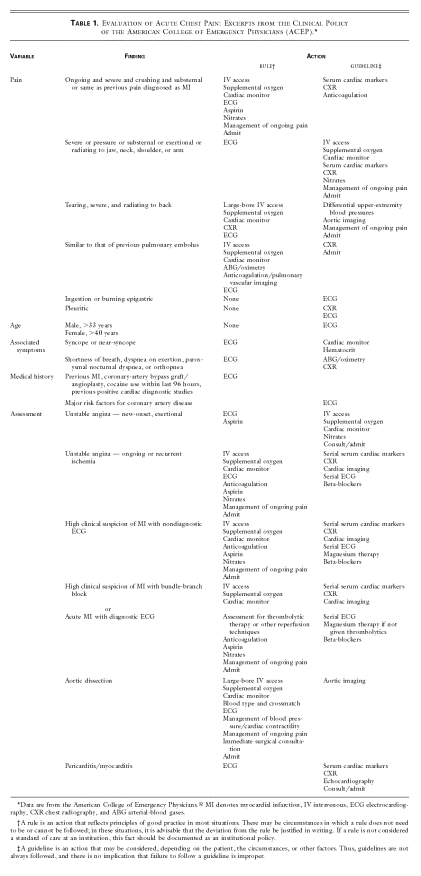
Chest pain
In a typical population of patients with acute chest pain who present at the emergency
department, approximately 15 percent have acute myocardial infarction and about 30 to
35 percent have unstable angina. Only 2.1 percent of patients with acute myocardial infarction
were discharged from the emergency department. In that population, the risk-adjusted mortality
was approximately double that of patients who had been admitted.
The prevalence of acute myocardial infarction was 80 percent among patients with1 mm or more
of new ST-segment elevation and 20 percent among patients with ST-segment depression or
T-wave inversion not known to be old.
In the absence of electrocardiographic changes consistent with the presence of ischemia, the risk
of acute myocardial infarction was 4 percent among patients with a history of coronary artery
disease and 2 percent among patients with no such history (unpublished data).
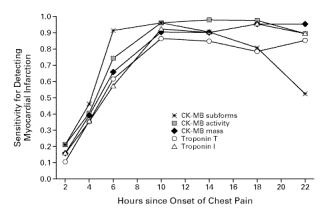
In a study of rapid assays for troponins T in 773 consecutive patients with acute chest pain but
no ST-segment elevation, 94 percent of the patients with myocardial infarction had a positive
result for troponin T within six hours after the onset of chest pain. The specificity was 89 percent.
The sensitivity of the rapid assay for detecting myocardial infarction ranged from 33 percent for
patients who presented within two hours after the onset of symptoms to 86 percent for patients
who presented after having symptoms for eight hours;
specificity ranged from 86 percent to 100 percent.
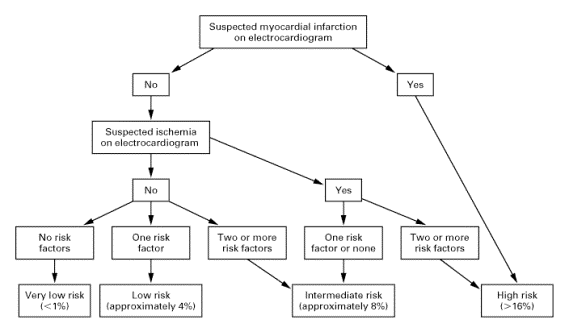
This algorithm had a sensitivity for detecting myocardial infarction that was similar to that of
the evaluating physicians' decisions with regard to admission to the coronary care unit (88
percent and 87.8 percent, respectively) and had a significantly higher specificity (74 percent vs.
71 percent).
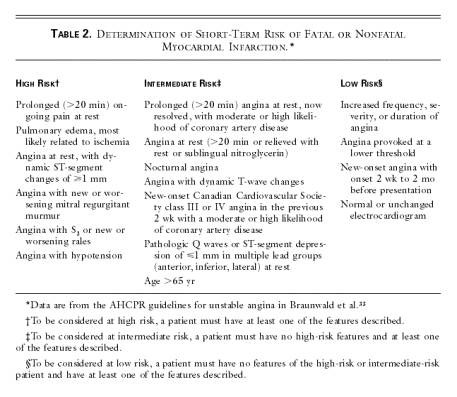
Syncope
・予後の悪い心疾患を見逃さない.
Syncope of unknown etiology carries a favorable prognosis with 1-year follow-up data showing
a low incidence of sudden death (2%), a 20% chance of recurrent syncope, and a 78% remission rate.
身体所見、心電図が正常で、45才以下なら外来でフォロー可能.
心不全や心室性不整脈の既往、異常心電図、45才以上なら救急外来で様子観察か、入院.
Anaphyraxis
入院の適応
ボスミンを使用した患者は全例最低6時間は観察し、この間無症状なら帰宅可.
遠方者やsevereな反応のあった者、高齢者なども考慮.
退院の適応、処方、外来予約
ボスミンを使用した患者は全例最低6時間は観察し、この間無症状なら帰宅可
原因薬剤がわかれば、(疑わしければ)薬剤名を持たせて帰宅.
抗ヒスタミン剤とPSL20-40mg4日間.
帰宅後に何か症状があれば、再来するように伝える.
特に問題なければフォローは不要だが、皮膚科受診の紹介や重症例は外来で一度フォローする.
Hemoptysis
Infectious nontubercular cause 25%
Tbc 5%
Neoplasia 28%
Cardiovascular 3%
Miscellaneous 13%
Undetermined 28%
Mild less than 5ml of blood in 24h
Moderate 5-600ml
Massive greater than 600ml
バイタルが異常なものは入院して様子観察.
バイタル、胸写ともに問題なければ外来で.
GI bleeding
5 poor prognostic factors in upper GI bleeding
Initial hematocrit less than 30%
Initial systemic blood pressure lower than 100mmHg
Red blood in the NG lavage
History of cirrhosis or ascites on exam
History of vomiting red blood
Most common source of massive lower GI bleeding is an upper GI site.
Diverticulitis 35%
Angiodysplasia 30%
Cancer polyp 10%
Rectal disease 7%
Other 3%
Undiagnosed 15%
80-90% lower GI bleeding will stop without therapy.
Suicide
SAD PERSONS score
Sex female 3times more likely to attempt,but men succeed 3times.
Age 19or younger and 45 or older are high risk
Depression 40-80% results from depression, 15% kill themselves
Previous attempt 64times risk
Ethanol abuse
Rational thinking loss functional psychosis command hallucination
Social support lacking
Organized plan
No spouse
Sickness
Discharge criteria
Crisis is identified and addressed
Patient has low SAD PERSONS score
Patient verbally “contacts” to return if condition worsens
Family member or friend agrees to stay with patient
Patient has a stable and supportive home environment
Telephone consultation with health care provider responsible for follow-up is performed
Follow-up appointment within 24-48 hours is scheduled.
TIA
入院.
Heat illness
軽い意識障害でも、急激に痙攀などおこることあり.解熱するまで様子観察.
Near drowning
重度の低酸素血症や、一過性でも意識障害があったものは入院して様子観察.
胸写、パルスオキシで異常なく、意識障害の既往もなければ帰宅可.
Electrical injury
全く何の症状がなくとも6-8時間はモニターして様子観察して帰宅.
何らかの症状があったり、どれぐらいの電力であったかが不明な場合は入院.
最終更新:2006年08月28日 00:19






